You can feel it before you can explain it.
Something has shifted. Maybe it’s the way they sound on the phone. Maybe it’s how quickly conversations end. Maybe it’s just a quiet, persistent fear that won’t let you rest.
As a clinician—and as someone who has sat across from many parents in this exact place—I want to say this first:
You are not overreacting. You are responding to something real.
If you’re trying to understand what kind of help might be appropriate right now, you can explore options like medical detox support while we walk through your most urgent questions together.
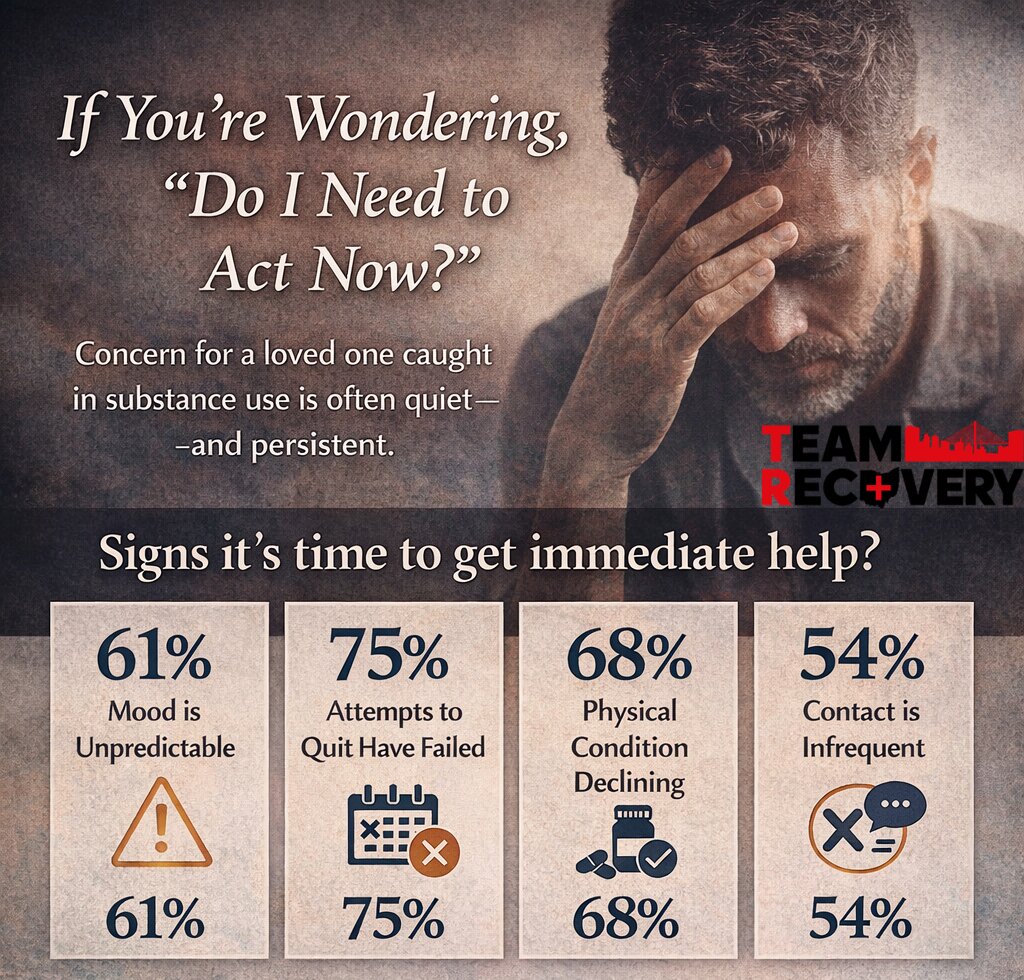
How do I know if this is serious enough to need immediate help?
Most parents I speak with are waiting for something undeniable.
A hospital visit. A legal issue. A moment where it’s obvious to everyone.
But what I’ve learned is this: the most important signals are often quiet.
It’s the repetition that matters:
- They said they were done—but they’re using again
- Their mood feels unpredictable or flat in a new way
- They’re harder to reach, harder to talk to
- You feel like you’re “losing” them in small, subtle ways
There’s a specific kind of tension parents carry here. It sounds like:
“What if I’m overreacting?”
“What if I wait too long?”
If you’re asking that question, you’re already paying closer attention than most.
You don’t need a crisis to justify concern. You just need a pattern.
What risks am I actually worried about?
Fear can feel overwhelming because it’s unclear.
Let’s ground it.
There are generally two types of risks parents are sensing:
1. Physical dependence
This is when the body has adapted to a substance. If use suddenly stops, the body reacts.
That reaction can range from uncomfortable… to medically serious.
2. Instability and unpredictability
This is often what keeps parents up at night.
Tolerance changes. Substances get mixed. What they’re taking may not be what they think it is.
Even people who “seem fine” can be at risk because the line between manageable and dangerous isn’t always visible.
This isn’t about assuming the worst.
It’s about recognizing that the body sometimes needs support to stabilize safely.
Can’t they just stop on their own?
This question carries so much hope—and so much frustration.
You’ve probably seen moments where they almost stopped. Maybe they did for a few days. Maybe even longer.
And that makes it even harder to understand why they can’t just… stay stopped.
Here’s the honest answer:
Sometimes they can’t—not without support.
Not because they don’t care. Not because they’re choosing this.
But because their brain and body have adapted in ways that make stopping feel overwhelming, even frightening.
I often tell parents this:
If willpower alone worked, most people wouldn’t get this far.
This isn’t a motivation problem. It’s a regulation problem—physical, emotional, neurological.
And that’s why early support matters.
What does safe support actually look like in the early stage?
In the beginning, the goal isn’t to fix everything.
It’s to stabilize.
That means helping your child get through the most physically and emotionally vulnerable phase safely.
That kind of support often includes:
- Medical oversight to monitor symptoms
- Help managing discomfort, anxiety, or sleep disruption
- A structured environment where they’re not navigating this alone
It’s not about locking them into a long-term plan.
It’s about creating a safer starting point.
Because once the body settles, the conversation changes.
Clarity comes back. Options feel less overwhelming. Resistance sometimes softens.
What if my child refuses help?
This is where most parents feel stuck.
You can see the risk. You want to intervene. And they say no.
It can feel like standing outside a locked door, knowing something isn’t right inside.
Here’s what matters most in this moment:
You don’t have to solve everything—but you do need to stay steady.
That can look like:
- Keeping communication open, even if it’s brief
- Being honest about what you’re seeing without escalating into arguments
- Setting boundaries that protect your well-being and theirs
- Repeating, calmly, that help is available when they’re ready
Sometimes the shift doesn’t come from one big conversation.
It comes from consistency.
From hearing the same calm message again and again:
“I’m here. I care. And I’m not going to pretend this is okay.”
Am I too late to make a difference?
No.
Even if it feels like you’ve already tried everything.
Even if they’ve relapsed.
Even if you’re tired in a way that’s hard to explain to anyone else.
You are not too late.
I’ve seen turning points happen after years of struggle.
Not because everything suddenly became easy—but because something changed in how support showed up.
Sometimes it’s timing.
Sometimes it’s the right level of care.
Sometimes it’s simply that the door stayed open long enough.
Your presence still matters. More than you think.
What’s the first step I should take right now?
You don’t need a perfect plan.
You need one next step.
That might be:
- Talking to a professional who understands both the medical and emotional side of this
- Learning what levels of care exist and when they’re appropriate
- Asking questions without committing to anything yet
You’re allowed to gather information before making decisions.
You’re allowed to not have all the answers today.
The most important thing is this:
Don’t carry this alone.
A quiet truth most parents don’t hear enough
There’s a kind of grief that shows up here that doesn’t have a name.
It’s not just fear.
It’s not just frustration.
It’s watching someone you love struggle in a way you can’t fix for them.
And still showing up anyway.
That matters.
Even on the days it feels like nothing is changing—something is.
Connection is being maintained. Possibility is being kept alive.
And sometimes, that’s what opens the door later.
FAQs Parents Often Ask in This Moment
How quickly should I act if I’m worried?
If something feels different or escalating, it’s okay to act sooner rather than later. You don’t need certainty—you need awareness. Early conversations can prevent more serious situations later.
What if they’ve already been through treatment before?
This is more common than people realize. Prior treatment doesn’t mean future help won’t work—it may just mean a different approach or level of care is needed this time.
Should I confront them directly about what I think is happening?
Yes—but gently. Focus on what you’ve observed, not accusations. For example: “I’ve noticed you seem really off lately, and I’m worried about you.” Keep the door open instead of trying to win the conversation.
How do I set boundaries without pushing them away?
Boundaries aren’t punishments—they’re clarity. You can say, “I love you, and I can’t support this behavior,” while still staying emotionally available. It’s a balance, and it’s okay if it takes time to find it.
What if I’m wrong?
Most parents aren’t. But even if you are, starting a conversation about safety, stress, or well-being is never harmful. It shows care—not control.
How do I take care of myself through this?
You matter in this too. Talk to someone you trust. Consider support groups or counseling for yourself. You don’t have to carry this silently.
There’s no perfect way to handle this. No script that guarantees the outcome you want.
But there is a way to stay present, informed, and connected—without losing yourself in the process.
And sometimes, that’s what makes all the difference.
Call 419-314-4909 or visit our medical detox support to learn more about our Medical Detox Program services in Toledo, Ohio.